I was honestly surprised by the many responses to my endometriosis article and by how strongly more visibility is desired, which is very understandable. And since endometriosis is also more often first diagnosed as depression when doctors do not know what to do next, it is only consistent that we now look at the topic of depression holistically as well.
Depression is not a sign of weakness, it is a state of alarm
Depression is still often reduced to a chemical imbalance in the brain, too little serotonin, or mental weakness. Such explanations sound simple, but they do not bring comfort, and they do not truly help those affected because they ignore physical causes.
Research and practice have long shown that depression is often a physical response, a state of alarm that the body sends when multiple systems fall out of balance. Chronic inflammation, hormonal dysregulation, changes in the gut microbiome, ongoing stress in the nervous system, and not being seen medically can trigger or intensify depressive symptoms.
Many women with endometriosis experience this directly. When pain and dysregulation are ignored, the diagnosis of depression is often made first, as a substitute diagnosis because no one else sees the underlying cause. In men and in people without endometriosis, the mechanisms are similar. The body sends signals that are often labelled as psychological instead of being understood as a warning system for physical dysregulation.
Gut, nutrition, and nutrients, the foundation for mood
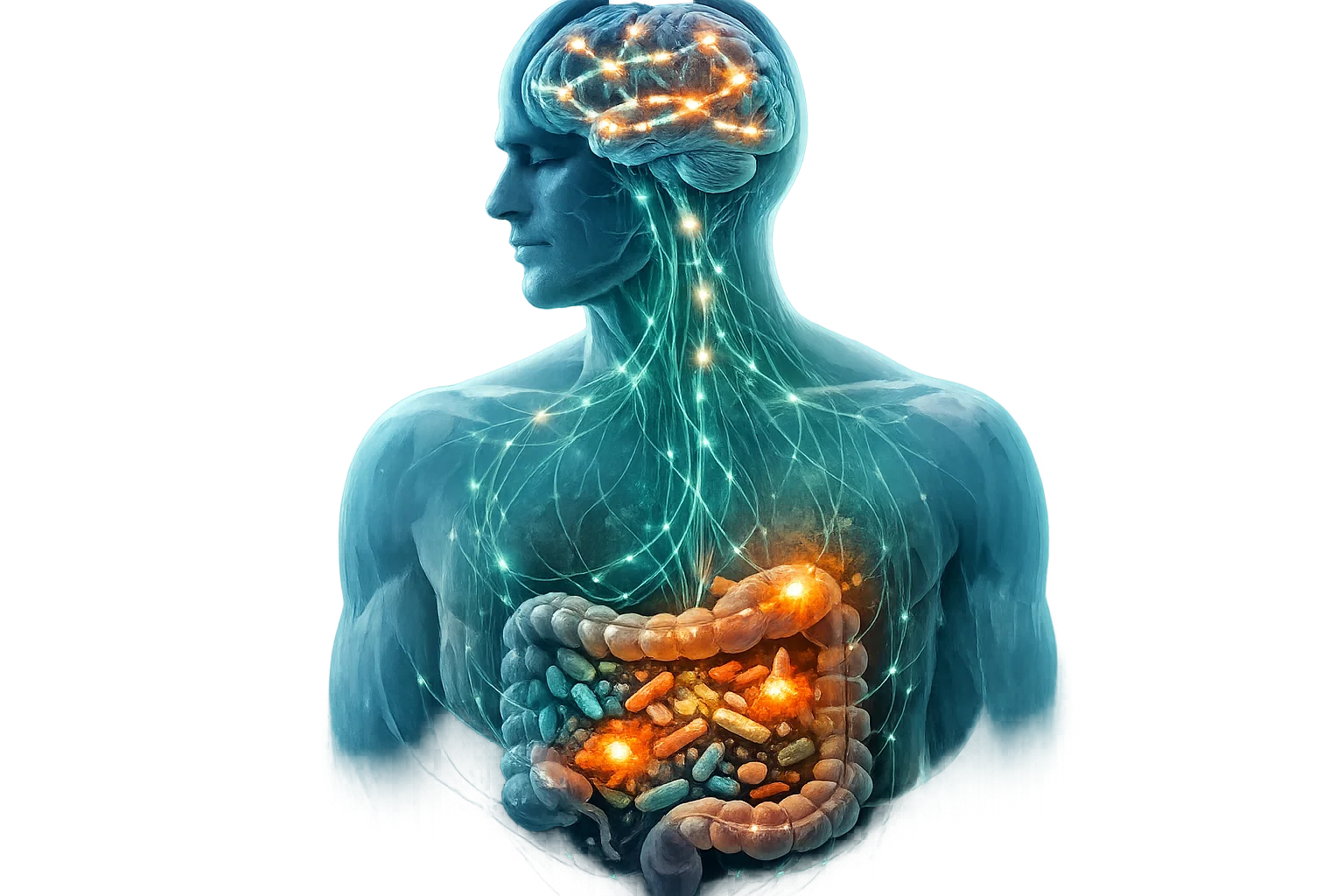
A central lever for depressive symptoms is the gut. Studies show that people who consume a lot of industrially processed foods, sugar, and fried foods have a significantly altered microbiome. This influences inflammation, neurotransmitters, hormones, and even the stress response.
- Serotonin production: 90 percent of serotonin is produced in the gut. A damaged microbiome means less raw material for serotonin and therefore less stability for mood, sleep, and motivation.
- Inflammatory processes: Sugar and trans fats promote silent inflammation. This acts directly on the brain, modulates neurotransmitters, and worsens stress resilience.
- Blood sugar fluctuations: Frequent sugar intake causes insulin spikes and drops. This strains the nervous system, increases fatigue and cravings, and can intensify depressive moods.
Anyone who wants to approach depression holistically must understand nutrition as a fundamental building block for healing, not just as a nice to have.
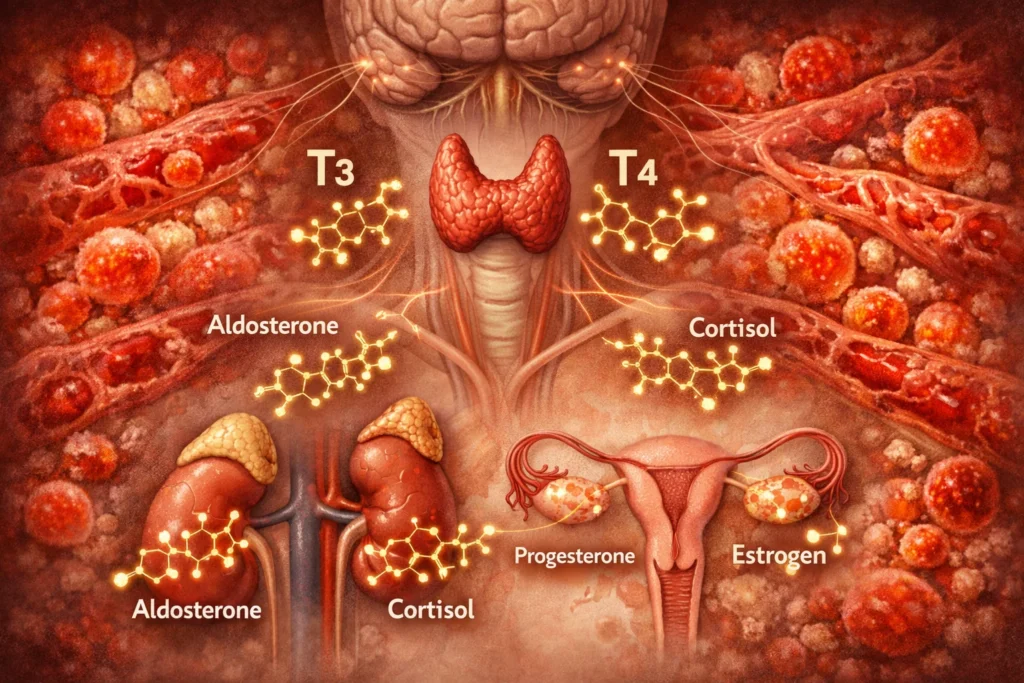
Hormonal dysregulation and chronic inflammation
Hormones do not only regulate reproduction, they also influence energy, stress response, sleep, and mood. An imbalance, whether in estrogen and progesterone, cortisol, or testosterone, can strongly affect depressive symptoms.
- Cortisol: Chronic stress increases cortisol, which in turn lowers progesterone. Progesterone has anti inflammatory effects and stabilises mood.
- Estrogen dominance: A relative excess of estrogen can destabilise mood, intensify inflammation, and disrupt sleep.
- Inflammation: Excess sugar, poor fats, lack of movement, and sleep deficiency create a chronic inflammatory state. Inflammatory markers such as CRP or interleukins are elevated in many people with depression.
Depression wird so zu einer körperlichen Reaktion auf systemische Dysbalance, nicht zu einem Zeichen von Charakterschwäche.
5-HTP: Natural support for serotonin
Before modern antidepressants existed, 5-HTP was used with the aim of increasing serotonin more directly. It crosses the blood brain barrier quickly and provides the body with a direct precursor for serotonin. Studies suggest that 5-HTP may help in mild to moderate depression and, in some comparisons, showed effects similar to early antidepressants, without the classic dependence potential.
Important: Anyone who is already taking antidepressants and is considering using 5-HTP alongside them should do so only in consultation with a physician. 5-HTP can raise serotonin levels and works directly, independent of the receptor pathways that many antidepressants influence. Taking antidepressants and 5-HTP at the same time can be dangerous because serotonin can rise too high, a condition known as serotonin syndrome. Symptoms can include agitation, tremor, a markedly increased heart rate, fever, sweating, muscle cramps, and in the worst case life threatening states. This is why the following applies: taper antidepressants gradually, and only then begin 5-HTP in a controlled way, always under medical supervision.
Nutrients that stabilize the brain and why the interplay matters
Before any intervention, including 5-HTP, a nutrient check should be done. Many neurotransmitters, hormones, and enzyme systems depend on each other. If even one building block is missing, others can only work to a limited extent.
- Magnesium calms the nervous system, helps regulate stress responses, and supports sleep quality.
- B1, B6, and B12 are essential for the production of serotonin, dopamine, GABA, and noradrenaline; without them, signals between nerve cells cannot be transmitted optimally.
- Zinc is important for neurotransmitter function, receptor activity, and hormonal balance; it supports the regulation of stress hormones.
- Iron is necessary for oxygen supply to the brain; deficiency can lead to fatigue, concentration problems, and reduced neurotransmitter production.
- Iodine plays a central role in thyroid hormones, which influence metabolism, energy, and mood.
- Folate is involved in the synthesis of serotonin, dopamine, and noradrenaline; it works synergistically with B12 and B6.
- Vitamin D helps regulate inflammatory processes, supports the immune system, and influences neurotransmitter receptors.
- Vitamin C is an antioxidant, protects nerve cells, and supports the conversion of dopamine to noradrenaline.
- Omega-3 fatty acids are essential for the cell membranes of nerve cells, have anti inflammatory effects, and influence signal transmission.
These nutrients work together: B vitamins function closely as a team, omega 3 fatty acids support an optimal membrane structure, vitamin D modulates inflammatory processes, and magnesium supports enzymes that activate neurotransmitters. An imbalance or deficiency can significantly limit the effectiveness of any therapy, whether 5-HTP, psychotherapy, or medication support.
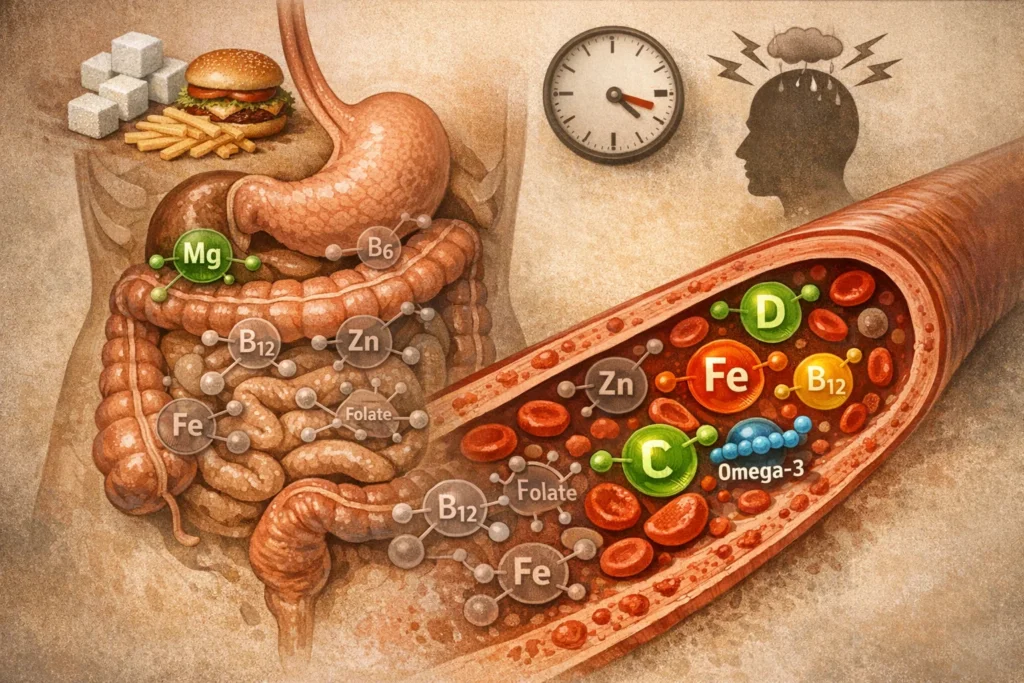
Causes of deficiency:
- Unfavorable diet (too much sugar, too little whole foods)
- Chronic inflammation or gut dysbiosis (can lead to reduced absorption)
- Medications (for example proton pump inhibitors, antidepressants, certain antibiotics)
- Chronic stress (increases demand and can reduce absorption)
- Genetic differences or hormonal imbalances
The consequence: When the balance of these nutrients is restored, the body’s own systems can become more stable, neurotransmitter production can be supported, and a foundation can be created for a more sustainable improvement in mood, whether additional medication is used or a holistic approach is chosen.
Antidepressants: effects and limitations
Antidepressants can be very helpful in many cases, especially when depressive symptoms are severe, but they mainly act on symptoms: they influence signal transmission in the brain and can stabilize mood and drive in the short term. At the same time, they do not address underlying causes such as chronic inflammation, hormonal imbalances, gut dysbiosis, or nutrient deficiencies.
Another important point, which many people are not aware of, is that antidepressants cannot be stopped abruptly without withdrawal symptoms. This means the body adapts to the medication, and a gradual taper under medical supervision is necessary. This phenomenon is sometimes incorrectly described as “addiction,” but more accurately: the body adapts to the substance, and stopping too quickly can lead to symptoms that should be medically monitored.
Lifestyle, stress management, and sleep: the underestimated levers
Chronic stress is a major amplifier in depression. It persistently activates the hypothalamic pituitary adrenal axis (HPA axis), which can lead to elevated cortisol. Chronically elevated cortisol can block nervous system recovery, inhibit neurogenesis in the hippocampus, and shift hormonal axes such as progesterone and estrogen or testosterone. Over time, this can contribute to sleep disturbances, low drive, cognitive problems, and a higher vulnerability to depressive episodes.
Sleep is not a luxury, it is a core part of recovery. During deep sleep phases, neurotransmitters such as serotonin and dopamine are regulated, the immune system is relieved, inflammation is reduced, and the brain is “cleansed”, processes that are significantly impaired with chronic sleep deprivation. Every hour of lost sleep can directly affect mood, concentration, irritability, and the ability to cope with stress.
Movement is another lever that is often underestimated. Even moderate physical activity, for example 20 to 30 minutes of brisk walking, cycling, or yoga, can support serotonin production, promote the growth of new nerve cells (neurogenesis), reduce inflammation, and improve blood sugar regulation. A mix of endurance, strength, and mindful movement can be particularly effective because different mechanisms in the brain are activated.
Stress management strategies are essential to break the cycle of overwhelm, sleep loss, and chronic inflammation. This includes:
- Breathing techniques and meditation can lower cortisol, improve heart rate variability, and promote relaxation.
- A structured daily routine with regular meals, movement, and sleep times supports stable biological rhythms.
- Social support, such as exchanging, being listened to, and feeling seen, can reduce stress and activate reward systems in the brain.
- Breaks and deliberate switching off, for example phone free time, contact with nature, hobbies, all of these can allow the nervous system to recover.
If you want to meet depression holistically, you should not neglect these factors. They are not “nice to have” extras, but central building blocks that directly influence neurotransmitter production, hormonal balance, gut function, and the immune system. A combination of stable sleep hygiene, regular movement, and targeted stress reduction can significantly increase the effectiveness of therapies, whether medication based, psychotherapeutic, or supported with nutrients.
Societal dimension and being seen
Depression often remains invisible. Many people continue to function in everyday life, hide their symptoms, and frequently experience that their suffering is not taken seriously. Comments such as “Don’t be so dramatic” or “You’ll be fine again soon” are something many encounter, even from those close to them. This subtle devaluation can intensify fear, shame, and isolation, and it is precisely this fear that keeps many from seeking help openly or speaking about their symptoms.
This persistent inner tension does not remain without consequences, because it keeps the body in a state of chronic alertness, in which stress hormones such as adrenaline and cortisol stay elevated. In the short term, this state can support survival, but with chronic activation it becomes a burden: it ties up energy, shifts metabolic priorities, and impairs many bodily processes, making regeneration, hormonal balance, neurotransmitter production, and even the effective use of available nutrients increasingly difficult. The body is then no longer operating in a mode of recovery, but in a mode of endurance, even when, objectively, sufficient resources might be present.
Feeling seen and taken seriously is therefore a central healing factor, almost as important as medical measures. When people experience that their body and mind respond to strain, that their symptoms are real and their experiences are valid, space opens for self care, re evaluation, and the willingness to take steps toward improvement.
Depression requires time, patience, and respect for the complexity of the human body, and it also calls for a shift in society: away from blame and performance pressure, and toward understanding, openness, and the recognition that psychological strain is a real response that is physically and biochemically understandable.
Are you interested in my topics and do not want to miss anything? Then subscribe to my Newsletter and you will receive interesting insights on “illnesses viewed holistically” in your inbox whenever a new blog post is published.
Sources
Gut, nutrition, and the microbiome:
The gut microbiome brain axis: how gut health can influence depression
https://jms.ump.edu.pl/index.php/JMS/article/view/1173
Nutrition, sugar, and fried foods in depression:
The association between diet quality, dietary patterns and depression in adults: a systematic review
https://link.springer.com/article/10.1186/1471-244X-13-175
Association of sugar consumption with risk of depression and anxiety: a systematic review and meta-analysis
https://link.springer.com/article/10.1186/s12888-024-05531-7
Association between junk food consumption and mental health problems in adults: a systematic review and meta-analysis
https://pubmed.ncbi.nlm.nih.gov/38867156
Serotonin production in the gut:
The Relationship Between the Serotonin Metabolism, Gut-Microbiota and the Gut-Brain Axis
https://pubmed.ncbi.nlm.nih.gov/31345143
Indigenous bacteria from the gut microbiota regulate host serotonin biosynthesis
https://pmc.ncbi.nlm.nih.gov/articles/PMC4393509
Hormonal imbalances and inflammation:
Meta analyses on HPA activity and depression: https://pubmed.ncbi.nlm.nih.gov/29150144/
Estrogen dominance and mood, hormonal influences on depression
Sex differences in depression: clinical perspectives
https://pubmed.ncbi.nlm.nih.gov/30601706
Premenstrual syndrome and premenstrual dysphoric disorder: definitions and diagnosis
https://pubmed.ncbi.nlm.nih.gov/31021735/
Mood, menopause, and hormones: evidence for treatment with estradiol
https://pubmed.ncbi.nlm.nih.gov/27047275/
Inflammation and depression: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4080723/
5‑HTP und serotonin:
Tryptophan and 5‑Hydroxytryptophan for depression https://pubmed.ncbi.nlm.nih.gov/11869656/
Systematic review and meta analysis on 5-HTP for depression
https://pubmed.ncbi.nlm.nih.gov/31504850
The Serotonin Syndrome: From Molecular Mechanisms to Clinical Practice
https://pmc.ncbi.nlm.nih.gov/articles/PMC6539562
Nutrients and neurotransmitters:
Zinc, magnesium, selenium, and depression: an overview of evidence, potential mechanisms, and implications https://pmc.ncbi.nlm.nih.gov/articles/PMC5986464/
Vitamin D supplementation for depressive symptoms: a systematic review and meta analysis of randomized controlled trials
https://pubmed.ncbi.nlm.nih.gov/24632894
Meta analysis and meta regression on supplementation with omega 3 polyunsaturated fatty acids in major depression
https://pubmed.ncbi.nlm.nih.gov/26978738
The association between folate and depression: a meta analysis
https://pubmed.ncbi.nlm.nih.gov/28759846
Antidepressants and tapering:
Antidepressant discontinuation syndrome https://pubmed.ncbi.nlm.nih.gov/38620563/
Stress, sleep, movement:
The HPA axis as a target in depression https://pubmed.ncbi.nlm.nih.gov/37581323/
Sleep deprivation, neurotransmitters, and mood:
Sleep deprivation and depression: a bidirectional relationship https://pmc.ncbi.nlm.nih.gov/articles/PMC4318605/
Exercise, neurogenesis, and depression:
Antidepressant like effects of exercise: evidence for an adult neurogenesis hypothesis https://pmc.ncbi.nlm.nih.gov/articles/PMC1413959/
Societal dimension, being seen:
Stigma toward depression and its influence on the intention to seek help
Social isolation and loneliness and their association with mental health and cognitive functionhttps://pubmed.ncbi.nlm.nih.gov/16403038/ Social isolation and loneliness and their association with mental health and cognitive function https://pmc.ncbi.nlm.nih.gov/articles/PMC9938924/