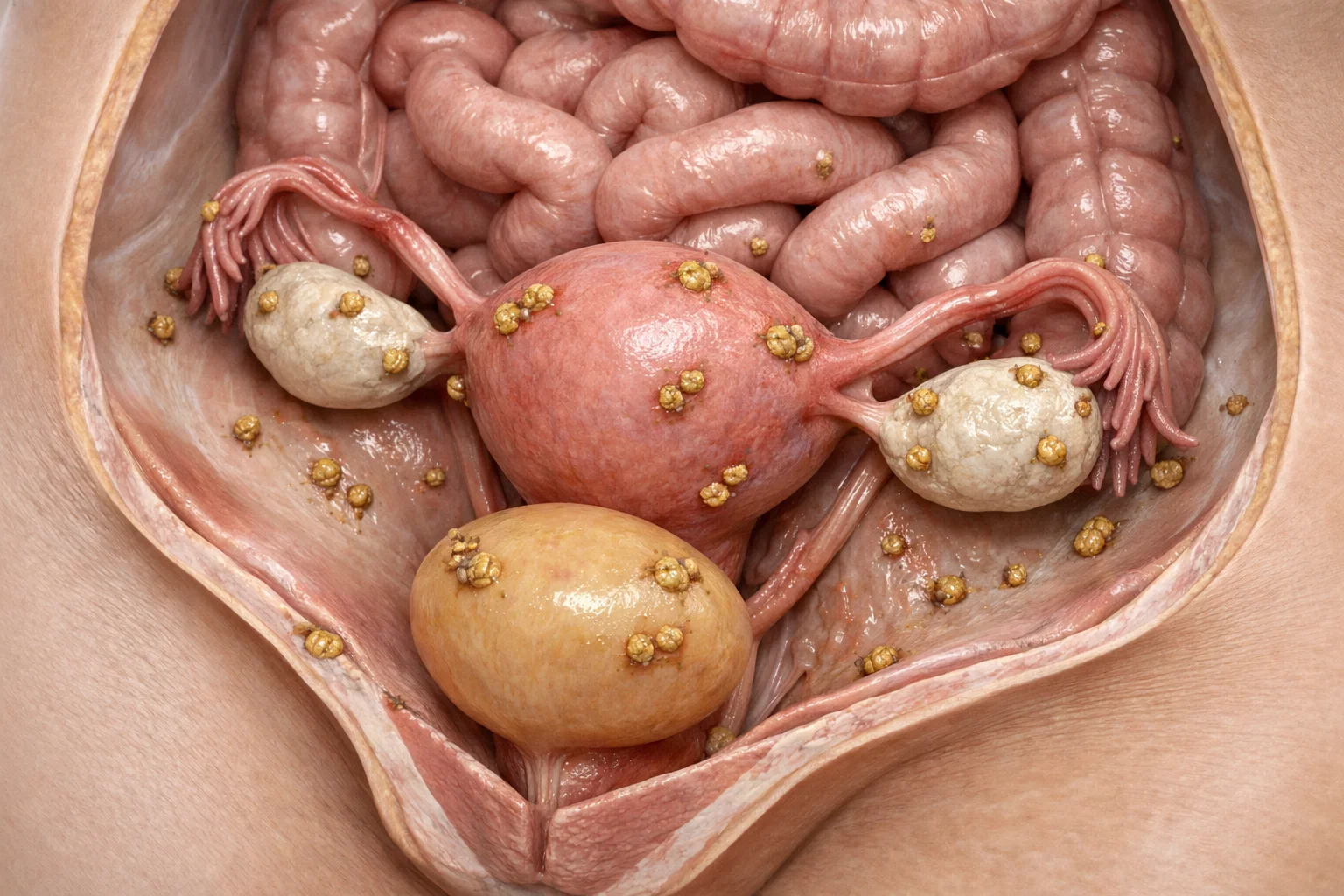
Endometriosis is not a whim of the body, it is a response to years of medical ignorance
Endometriosis is not a rare condition
Endometriosis is not a rare condition, even if it is still treated as if it were. Estimates suggest that one in ten women of reproductive age is affected, and some studies even report higher numbers. And yet, on average, seven to ten years pass before a diagnosis is made. Years in which pain is normalised, symptoms are downplayed, and women repeatedly hear: This is just your period, You just have to get through it, This is psychosomatic.
Endometriosis is therefore not only a medical condition, but also a social one, one that shows how little space women’s reality of pain is still given today.
Medical definition versus systemic reality
Medically, endometriosis describes the presence of tissue similar to the lining of the uterus outside the uterus, for example on the ovaries, fallopian tubes, intestines, bladder, peritoneum, or even in more distant locations. This tissue responds to hormonal fluctuations, especially estrogen, and can cause cycle related inflammation, swelling, adhesions, and severe pain.
But this definition falls short. Endometriosis is not a purely gynaecological condition, it is a systemic inflammatory disease with hormonal, immunological, metabolic, and neural involvement.
Symptoms beyond the pelvic area
Many affected people do not only suffer from severe menstrual pain, but also from chronic lower abdominal pain, back pain, digestive problems, bloating, diarrhoea or constipation, pain during sex, cycle irregularities, exhaustion, brain fog, mood swings, and not infrequently from unfulfilled desire to have children. Nevertheless, these symptoms are often viewed and treated in isolation instead of being understood as the expression of a shared system that has fallen out of balance.
Hormonal suppression versus treating causes
A central element in conventional medical treatment to this day is hormonal suppression of the cycle, usually in the form of the contraceptive pill or other progestins. The logic behind it is simple. If the cycle is switched off, there are fewer hormonal fluctuations, fewer bleedings, and less pain. For many women, this can indeed bring short term relief. But this strategy treats symptoms, not causes, and it is not without consequences.

The contraceptive pill as an endocrine intervention
The contraceptive pill acts as a major intervention in the hormonal system. It suppresses the natural cycle, changes communication between the brain, ovaries, and adrenal glands, and affects the liver, gut, and microbiome. Barbara O’Neill and other holistic practitioners have pointed out for years that hormonal contraceptives can act as endocrine disruptors. This does not mean that every woman develops endometriosis because of the pill, but it can intensify existing dysregulation and create unfavourable conditions.
Estrogen and estrogen dominance
Estrogen plays a key role in endometriosis. Endometriosis lesions are often estrogen sensitive, they grow and become inflamed under its influence. At the same time, many affected people show signs of so called estrogen dominance, not necessarily in the sense of an absolutely high estrogen level, but a relative excess in relation to progesterone. The pill changes precisely this ratio. It provides synthetic hormones that suppress the body’s own progesterone and override natural regulation. In addition, it affects the liver, which is responsible for breaking down excess hormones, and the gut, through which a large portion of these hormones is excreted.
Gut health and the estrobolome
This is where an often overlooked connection comes into play: the gut. The gut is not only a digestive organ, but also a central hormonal and immunological control centre. Through the so called estrobolome, a group of gut bacteria, it is also determined how much estrogen is reactivated or excreted. A disturbed gut flora can lead to estrogen that has already been broken down being reactivated and sent back into circulation. The result is an increased hormonal burden that can promote inflammatory processes.

Nutrition as a long term influencing factor
Nutrition plays a decisive role in this context, not as a quick fix, but as a long term influencing factor. Many dietary habits of our time have a quietly pro inflammatory effect, place a hormonal burden, or irritate the gut. This includes in particular high sugar consumption. Sugar influences insulin, insulin influences inflammatory processes, and inflammation is a central element of endometriosis. In addition, sugar changes the composition of the microbiome, promotes certain bacterial groups and displaces others, which in turn can influence estrogen metabolism.
Alcohol, the liver and inflammation
Alcohol is also often underestimated. It burdens the liver, precisely the organ responsible for breaking down hormones. Regular alcohol consumption can lead to estrogen being broken down more slowly and remaining in the system longer. At the same time, alcohol increases intestinal permeability, promotes low grade inflammation, and can intensify pain. A single glass may seem harmless, but with a condition that responds to cumulative burdens, the overall sum matters.
Fats and inflammation
Another factor is the quality of the fats consumed. Trans fats, heavily processed vegetable oils, and an unfavourable ratio of omega 6 to omega 3 fatty acids promote inflammatory processes. Many affected people report improvements, however, when they pay attention to anti inflammatory fats, for example from olive oil, avocado, nuts, seeds, and high quality omega 3 sources.
Gluten and the gut barrier
Gluten is also increasingly discussed in the context of endometriosis. Not because endometriosis is coeliac disease, but because gluten can affect the gut barrier in some women and can trigger immunological reactions. Studies show that a portion of endometriosis patients benefit from a gluten reduced or gluten free diet, especially when digestive complaints are present at the same time. This is not a dogma, but it is worth an individual trial.
A shift in perspective instead of symptom treatment
What can help is a shift in perspective. Away from the question How do we switch off the cycle and toward Why is this system reacting so strongly. Endometriosis does not develop overnight. It develops within a milieu of inflammation, hormonal imbalance, immunological dysregulation, and often years of overload. Stress also plays a role. Chronic stress influences cortisol, cortisol influences progesterone, and progesterone has anti inflammatory effects. When this balance becomes unstable, symptoms can intensify.
Holistic approaches: nutrition, gut, stress and lifestyle
From a holistic perspective, support for endometriosis therefore does not mean only pain medication or hormones, but an interplay of nutrition, gut health, stress regulation, sleep, movement, and a more conscious approach to hormonal interventions. Not every woman has to demonise the pill or stop it immediately, but every woman should be able to make an informed decision and understand the connections.
Social dimension and invisibility
The social dimension is also particularly important. Endometriosis is often made invisible because it is not always visible from the outside. Women keep functioning, go to work, take care of family, while fighting internally. Pain is normalised, suffering is individualised. What is needed is more education, more research, and above all more listening.
Final thoughts: seeing holistically, not only treating
Endometriosis is not a women’s disease that you simply have to accept. It is a signal from the body that something has fallen out of balance. Taking this signal seriously does not mean rejecting conventional medical measures across the board, but rather complementing them, questioning them, and placing them in a broader context.
A holistic perspective does not mean alternative instead of medical, but comprehensive instead of reduced.
Perhaps the most important step for many affected people is not the perfect diet or the one supplement, but the feeling of finally being seen. Understanding that their pain is real, that their body is not exaggerating, and that healing is often a process, not a quick intervention.
Endometriosis requires time, patience, and respect for the complexity of the female body, something that we as a society urgently need to relearn.
Sources
- Endometriosis as a systemic inflammatory disease
https://pubmed.ncbi.nlm.nih.gov/33640070
(Endometriosis as a chronic inflammatory disease: clinical challenges and systemic characteristics)
2. Role of estrogen and estrogen dominance
https://pmc.ncbi.nlm.nih.gov/articles/PMC7215544
(Hormonal regulation and endometriosis progression as well as the estrogen dependence of endometriosis lesions)
3. The contraceptive pill and hormonal disruption
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8353973/ (Oral contraceptives and long term hormonal effects)
https://www.frontiersin.org/articles/10.3389/fendo.2020.00252/full Endocrine disruptors and hormonal diseases)
https://pubmed.ncbi.nlm.nih.gov/32711116/ (Hormonal contraception and changes in the immune system)
https://pubmed.ncbi.nlm.nih.gov/32711116/
4.Gut, microbiome and the estrobolome
(https://pubmed.ncbi.nlm.nih.gov/34718567/ The role of gut and genital microbiota and the estrobolome in endometriosis, infertility and chronic pelvic pain
https://pubmed.ncbi.nlm.nih.gov/40692689
Impact of gut microbiota on endometriosis: linking physical injury to mental health
https://www.frontiersin.org/journals/microbiology/articles/10.3389/fmicb.2025.1552134/full
Association between endometriosis and gut microbiota: systematic review and meta-analysis
5. Nutrition, sugar and inflammation
https://pubmed.ncbi.nlm.nih.gov/36875844
Nutrition in the prevention and treatment of endometriosis: A review
https://pmc.ncbi.nlm.nih.gov/articles/PMC10967113
Causal effects of glycemic traits and endometriosis: a bidirectional and multivariate mendelian randomization study
6. Alcohol, the liver and hormone breakdown
https://journals.viamedica.pl/ginekologia_polska/article/view/103148
The influence of ethanol consumption on a course of endometriosis
7. Gluten, the gut barrier and endometriosis
https://impact.ed.ac.uk/research/endometriosis-research-shows-changing-diet-may-help
Improvement of endometriosis symptoms through, among other things, a gluten free diet
https://pmc.ncbi.nlm.nih.gov/articles/PMC11959439
Dietary Modification and Supplement Use For Endometriosis Pain
8. Omega 3, anti inflammatory effects and pain
Effect of omega-3 polyunsaturated fatty acid on endometriosis
9. Stress, cortisol & progesterone
https://www.researchgate.net/publication/38082762_Sex_Hormones_and_Mood_in_the_Perimenopause
Sex Hormones and Mood in the Perimenopause ((Schmidt PJ, Rubinow DR. Ann N Y Acad Sci. 2009;1179:70–85)
https://www.sciencedirect.com/science/article/abs/pii/S1567576924004600
Stress, pain, anxiety, and depression in endometriosis–Targeting glial activation and inflammation
10. Delayed diagnosis and the social dimension
https://www.liebertpub.com/doi/10.1177/15409996251380129
Endometriosis Diagnostic Delay and Its Correlates: Results from the ComPaRe-Endometriosis Cohort
https://pmc.ncbi.nlm.nih.gov/articles/PMC11106211
Loneliness and Perceived Social Support in Endometriosis: The Roles of Body Image Disturbance and Anticipated Stigma